Research
[Infection Control & Hospital Epidemiology] Escalating infection control response to the rapidly evolving epidemiology of the Coronavirus disease 2019 (COVID-19) due to SARS-CoV-2 in Hong Kong
Infection Control & Hospital Epidemiology, 20 March 2020
Vincent C.C. Cheng, Shuk-Ching Wong, Jonathan H.K. Chen, Cyril C.Y. Yip, Vivien W.M. Chuang, Owen T.Y. Tsang, Siddharth Sridhar, Jasper F.W. Chan, Pak-Leung Ho and Kwok-Yung Yuen
Highlights:
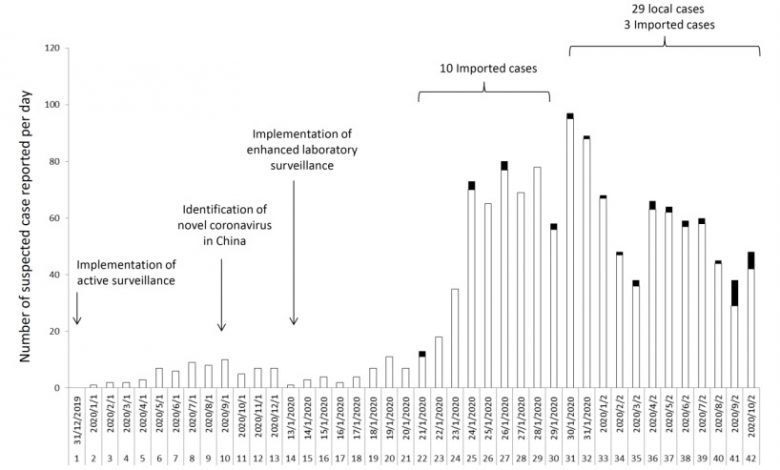
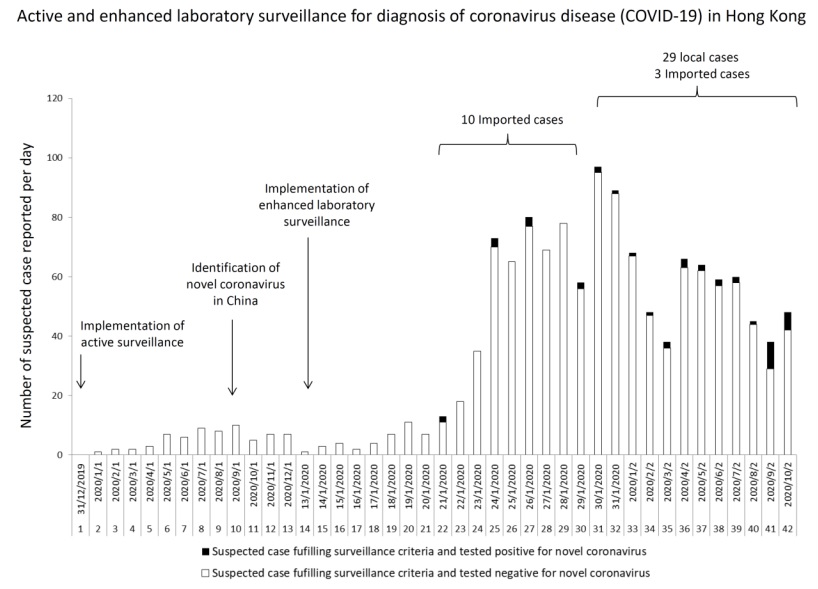
- To describe the infection control preparedness for Coronavirus Disease (COVID-19) due to SARS-CoV-2 [previously known as 2019-novel coronavirus] in the first 42 days after announcement of a cluster of pneumonia in China, on 31 December 2019 (day 1) in Hong Kong.
- A bundle approach of active and enhanced laboratory surveillance, early airborne infection isolation, rapid molecular diagnostic testing, and contact tracing for healthcare workers (HCWs) with unprotected exposure in the hospitals was implemented.
- The number of locally acquired cases significantly increased from 1 (7.7%) of 13 [day 22 to day 32] to 27 (93.1%) of 29 confirmed case [day 33 to day 42] (p<0.001).
- Twenty-eight patients (66.6%) came from 8 family clusters. Eleven (2.7%) of 413 HCWs caring for these confirmed cases were found to have unprotected exposure requiring quarantine for 14 days
- Environmental surveillance performed in a patient with viral load of 3.3×106copies/ml (pooled nasopharyngeal/ throat swab) and 5.9×106 copies/ml (saliva), respectively.
- Transmission within family remained a concernas 66% of confirmed cases (28 patients came from 8 family clusters) diagnosed in Hong Kong were spread among their family members.
- With the implementation of active and enhanced surveillance with progressive widening of screening criteria during the evolution of epidemic, we could recognize most of the confirmed cases upon hospitalization.
- Vigilance in hand hygiene practice, wearing of surgical mask in the hospital, and appropriate use of PPE in patient care, especially performing AGPs are the key infection control measures to prevent nosocomial transmission of SARS-CoV-2 evenbefore the availability of effective antiviral agents and vaccine.
Read full article

![Photo of [Nature Microbiology] Metallodrug ranitidine bismuth citrate suppresses SARS-CoV-2 replication and relieves virus-associated pneumonia in Syrian hamsters](https://fightcovid19.hku.hk/content/uploads/2020/10/Image-2-390x220.jpg)
![Photo of [Cell Reports Medicine] Oral SARS-CoV-2 inoculation establishes subclinical respiratory infection with virus shedding in golden Syrian hamsters](https://fightcovid19.hku.hk/content/uploads/2020/10/fx1_lrg-e1601870075235-390x220.jpg)